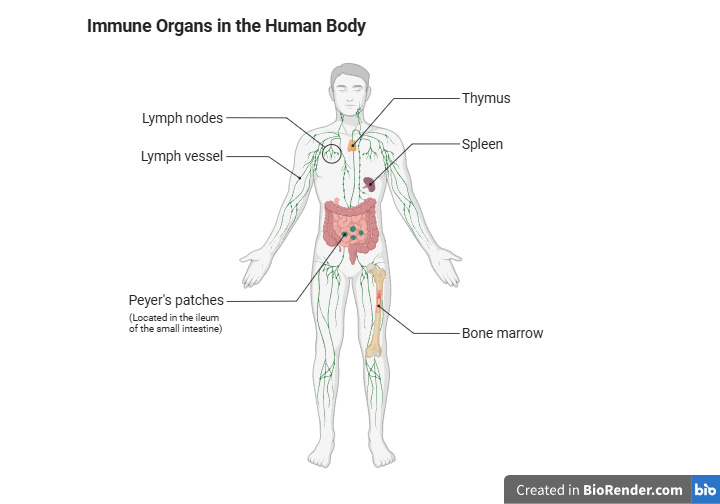
What Echinacea Actually Does (and the Immune System Physiology That Explains Why)
where the innate and adaptive arms hand off, why it matters, and where echinacea actually fits in.

Hey friends!
I promised you wild lettuce this week, and wild lettuce is not what’s landing in your inbox. The species sprawls in ways that deserve more attention than I could give it, the human studies on Lactuca virosa are thin in the places I most wanted them thick, and after a week that asked a lot of me for reasons I’m going to keep off the page, the idea of producing that monograph on the deadline I’d set for myself stopped being realistic. I didn’t want to leave you with silence, and I’m already so late with this post, so I’m reaching into the coursework folder and pulling out an assignment I actually liked.
I’ve cleaned it up, added a closer on the most-researched immune herb in the Western materia medica, and put the whole thing here for you.
I’m not sure if the wild lettuce piece will come. I’m hitting a lot of resistance with it and maybe that means it’s just not for me to write. So, why fight it and write a piece I’m not fully present in. You know? I hope that’s okay. I’m really sorry.
Anyways, here’s what we’re covering today:
How the body’s three layers of defense are actually structured (the barriers, the innate response, and the adaptive response)
What macrophages and the rest of the innate cells are doing in those first minutes after an invader gets past the barriers
How the adaptive immune system gets called in when the innate response isn’t enough, and how it builds the memory that protects you for years afterward
Where the two arms differ in speed, specificity, and memory, and why that distinction shapes how everything else works
The bridge between innate and adaptive immunity, where dendritic cells essentially teach the adaptive system what kind of response to mount (this is the most beautiful piece of the architecture, in my opinion)
What happens when the system fails, through immunodeficiency, hypersensitivity, and autoimmunity
A closing look at echinacea, the most-researched immune herb in the Western materia medica, and where its mechanism actually fits in the framework we just built
At the end of this, I want you to be able to look down at a splinter poking out of your skin, or take internal stock of exactly what's happening during a pesky cold, and actually narrate it to yourself. "My B cells are working hard replicating these antibodies right now." "My macrophages are eating some delicious gunk right now." :) That kind of thing.
Alright. The immune system, on a cellular level. Let’s get into it.

The Body’s Layered Defense
Most of what gets sold to you as immune support assumes the immune system is a single thing, one knob you can turn up or down, one circuit you can stimulate. The actual architecture is layered, redundant, and gorgeous in a way that I think gets lost in the supplement-aisle version of the story. It’s an intricate dance.
Your body keeps invaders out through three coordinated tiers, each with its own primary role in the larger response (Sompayrac, 2022):
The physical barriers, which keep most invaders out entirely before any cellular response ever has to happen
The innate immune system, which mounts a fast, broad response when those barriers are breached
The adaptive immune system, which builds a slower, more precise response tailored to the specific invader and remembers it afterward
The handoff between these layers is where most of the real intelligence in this system lives, and that handoff is the part of the story I want to spend the most time on today.
Here's what I want you to sit with for a second, because the layering itself is the point. Every tier of this system is doing intentional work, with each layer covering what the others can't quite reach and the gaps in one filled by the strengths of another. Even the old textbook line that the innate arm has no memory has started to soften in the last decade or so, as researchers have found that some innate cells can in fact be primed for stronger responses on subsequent exposures (more on that in a minute). The shape of the whole thing is intentional, and the more closely you look at it, the more obvious that becomes.
The First Lines: The Innate Immune System
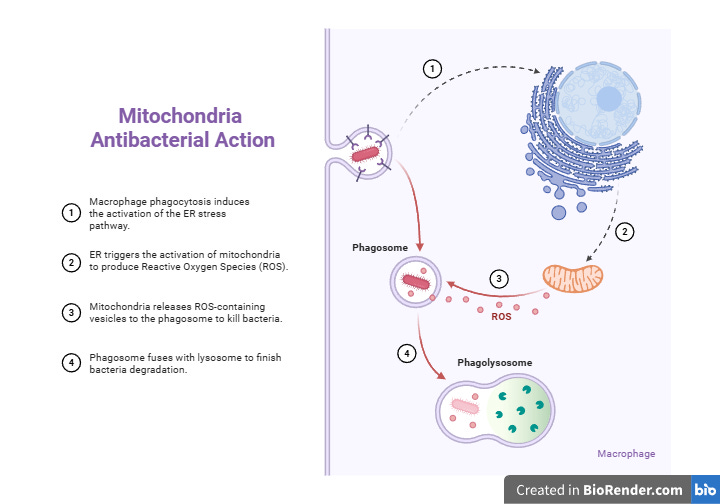
Once something has gotten past your barriers and is loose in the tissue, the first cells likely to encounter it are macrophages. They sit in tissues throughout your body, ready to recognize what doesn’t belong, and they do this using surface receptors tuned to pick up specific fats and carbohydrates that pathogens carry on their surfaces, the so-called “danger molecules” (Sompayrac, 2022). When a macrophage recognizes one of these patterns, it engulfs the pathogen into a phagosome, which then fuses with a lysosome packed with enzymes and reactive chemicals that destroy the invader from the inside. This whole process is called phagocytosis, and it’s happening in your body constantly, mostly without your awareness (Sompayrac, 2022).
While the macrophage is doing the eating, it’s also doing the talking. As it engulfs the pathogen, it secretes cytokines, which are hormone-like messengers that coordinate communication between immune cells and signal for the inflammatory response to begin (Sompayrac, 2022).
Inflammation has been miscast as a villain in a lot of the wellness conversation, when in practice it’s the recruitment mechanism the body uses to pull additional players to the site of trouble. The redness, the heat, the swelling, all of it is the body actively mobilizing, calling in neutrophils, which are the most abundant phagocytes in circulation, and natural killer cells, which target host cells that have already been compromised by viruses or other stressors. In parallel, the complement system activates, a cascade of plasma proteins that marks pathogens for destruction and amplifies the recruitment of immune cells to the site (Wang et al., 2024).
This entire response can mount within minutes to hours, and for most everyday encounters with pathogens, it’s enough. The infection is contained at the site, the affected tissue heals, and you never have any sense that anything happened.
The rest of this piece is for paid subscribers. Below the paywall, I cover how the adaptive immune system gets called in when the innate response isn’t enough, the bridge between the two arms where dendritic cells essentially teach the adaptive system what kind of response to mount (this is the most beautiful piece of the architecture, in my opinion), what happens when the system fails through immunodeficiency, hypersensitivity, and autoimmunity, and the full closing section on echinacea, including the caveat about who I’d hesitate to give it to, the mechanism mapped onto the innate response, and traditional preparation notes.
If you’ve been finding value in this work, please consider upgrading to support it. Paid subscribers also get access to the Materia Medica index and the Body Systems index, both of which are building out into a real working library you can use alongside your own practice.